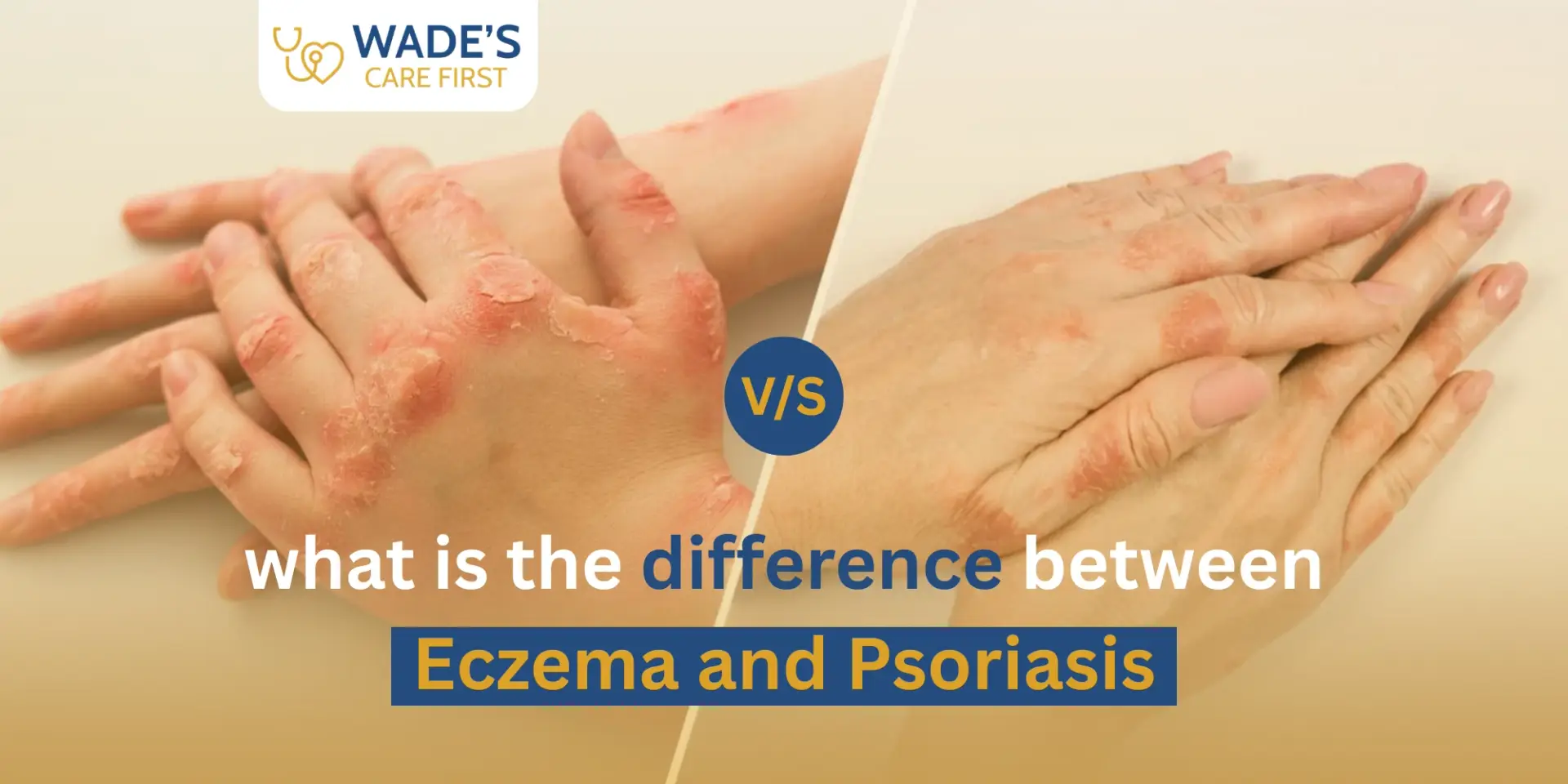
People mix these two up all the time – and honestly, it’s not hard to see why. They both result in red and irritated skin. They both have a tendency to flare and relax.
They can both get you scratching in the middle of the night and searching for answers during the day.
However, they are not alike and trying to treat them as one will most likely lead nowhere.
Eczema and psoriasis are distinct and different in nature, appear differently under a microscope, appear on various body parts, and react to varying therapies.
That difference counts a lot when one is attempting to feel good.
What follows is a plain-language breakdown of both conditions – what they are, how to tell them apart, who tends to get them, and what you can actually do about them.
Eczema
The skin of healthy people possesses a protective layer – a barrier that contains moisture and excludes irritants. The barrier does not work well in individuals with eczema.
Moisture is lost too readily, and the skin is sensitive to many things that would not bother a typical person: laundry detergent, change of temperature, a pet, even to sweating.
These irritants are then overreacted by the immune system leading to inflammation in the skin.
The consequence is the red and itchy and occasionally weeping rash that most people relate to the condition.
Eczema begins early – it may begin at a young age, as early as the first years of life – but it can also be developed by a person in adulthood, and a large number of individuals have it during childhood and carry it into adulthood.
What eczema actually looks like
- Patches of dry, intensely itchy skin that can feel raw or almost painful
- Redness that deepens after scratching
- Skin that weeps a clear fluid or crusts over when a flare is active
- Thick, leathery areas where the same spots get scratched repeatedly over time
- Small raised bumps that break open when scratched
- Itching that almost always peaks at night
What sets eczema off
The condition is not caused by one thing, but two primary factors are genetics and the environment working against each other.
- Your risk increases significantly in case of a family history of eczema, asthma, or hay fever.
- An alteration in the filaggrin gene undermines the skin barrier on a structural level.
- Ordinary irritants comprise perfumed soaps and laundry detergents, dust mites, pet dander, pollen, artificial fabrics, and perspiration.
- Drastic changes in emotions and weather, cold, dry air, in particular, can push the skin to the brink.
Psoriasis
Psoriasis is a different kind of problem. Instead of a barrier that doesn’t hold, the issue here is an immune system that has gone off-script.
It sends signals, making the skin cells multiply at an extremely rapid rate – days rather than weeks.
The skin is unable to dispose of the cells at the same rate as they accumulate on the surface, creating the thick, scaly plates that characterize the condition.
Psoriasis unlike eczema, is an autoimmune disease, that is, the body is attacking itself.
Such a difference goes beyond skin – psoriasis may affect the joints, nails and in some studies, even be associated with a greater risk of heart disease in uncontrolled long-term.
Psoriasis may manifest in adulthood, often at two intervals and these include individuals during the late teens to mid-30s years and later during 50-60 years.
What psoriasis actually looks like
- Raised, well-defined plaques covered in a thick silvery or white scale
- Skin underneath the plaques that’s red and sometimes bleeds when the scale is removed
- A burning or tight sensation around affected areas
- Nails that pit, thicken, crumble, or separate from the nail bed
- Itching that ranges from barely noticeable to genuinely disruptive, depending on the person
- Swollen, stiff, or painful joints – a complication called psoriatic arthritis – in some cases
What triggers psoriasis
- A parent or sibling with psoriasis is one of the strongest risk factors
- Strep throat – even a mild case – can kickstart a flare, especially a type called guttate psoriasis
- Stress is a consistent trigger for most people with the condition
- Certain medications, including some blood pressure drugs and mood stabilizers, are known to worsen it
- Smoking and heavy drinking both increase flare frequency and severity
- Skin injuries – a cut, a sunburn, a scratch – can cause psoriasis to appear at that exact spot (this is called the Koebner phenomenon)
| Psoriasis is not contagious. It is entirely internal – an immune system issue, not something that spreads from skin contact. |
Comparing the Two Directly
The easiest way to see the differences clearly is side by side.
| Eczema | Psoriasis | |
| What drives it | Skin barrier failure + immune overreaction | Autoimmune — immune cells attack healthy skin |
| What it looks like | Red, weepy, crusty; skin may crack and ooze | Raised, thick plaques with a silver-white scale |
| Itch | Severe and relentless, often worse at night | Varies — present but generally milder |
| Common onset | Infancy or early childhood; can start as adult | Late teens to mid-30s, or again around 50–60 |
| Favored locations | Skin creases, face, neck, wrists, ankles | Outer elbows, knees, scalp, lower back, nails |
| Nails affected? | Occasionally | Yes — pitting, thickening, or discoloration |
| Joint involvement | Rare | Yes — psoriatic arthritis in roughly 30% |
| Common triggers | Soaps, allergens, sweat, heat, stress | Stress, strep, skin injury, certain medications |
| Is it contagious? | No | No |
The Location Question: Where Each One Tends to Show Up
Location is often the single most useful clue. Both conditions can technically appear anywhere, but each has strong preferences.
Where eczema tends to settle
- The inner creases of the elbows and the backs of the knees – the fold, not the outside
- The face, especially in infants and young children – cheeks, around the eyes, the chin
- Wrists, ankles, and the backs of the hands
- The neck and collarbone area
- Skin folds where heat and friction build up
Where psoriasis tends to settle
- The outer surfaces of the elbows and knees – the bony part, not the crease
- The scalp, often with a clear boundary just past the hairline
- The lower back and tailbone area
- Palms and the soles of the feet, sometimes alone
- Nails, genitals, and under the breasts or in the skin folds in certain types
One pattern worth keeping in mind: eczema likes to hide in the folds. Psoriasis tends to show up on surfaces that take impact. Neither one is absolute, but location alone can often point a provider strongly in one direction during an exam.
Getting the Diagnosis Right
No blood test says “eczema” or “psoriasis.” Diagnosis is a clinical process – it comes from a provider who looks closely at the skin, asks detailed questions, and factors in your history.
One thing worth knowing: in people with darker skin tones, both conditions may look quite different from what appears in textbooks and online photos.
Can You Have Both at the Same Time?
You can, though it is uncommon. When both conditions occur together, they often appear in different areas. eczema in the creases, psoriasis on the outer surfaces – which can make each
Treatment: Why Getting the Diagnosis Right Comes First
The most important reason to distinguish between eczema and psoriasis is treatment. The approaches overlap in some areas but diverge significantly in others, and using the wrong one doesn’t just fail – it can sometimes make things worse.
How eczema is managed
- Daily moisturizing – not once in a while, but every day, especially right after a shower while the skin is still slightly damp
- Dupilumab (Dupixent) and other newer biologics for moderate-to-severe cases that don’t respond to topical treatment alone
- Antihistamines to help with sleep when nighttime itching is severe
- A detailed trigger audit – often the most productive and least discussed part of eczema management
How psoriasis is managed
- Coal tar preparations for scalp psoriasis and thicker plaques on the body
- Phototherapy – carefully controlled UV light exposure
- Oral medications
- Biologics – including TNF inhibitors and IL-17 or IL-23 blockers – which have genuinely changed the outcome for people with moderate-to-severe psoriasis
- Lifestyle changes – quitting smoking, limiting alcohol, managing weight and reducing chronic stress all make a measurable difference in how often and how badly it flares
| Biologics have changed what is achievable for both conditions. If you have been trying the same treatments for a long time without results, a conversation about whether biologics are appropriate for your situation is worth having. |
When to Stop Waiting and See Someone
Skin conditions have a way of getting rationalized. It’s just dry skin. It’ll pass. It’s probably nothing. And sometimes it does pass. But there are situations where waiting makes things harder, not easier.
Some clear reasons to book an appointment:
- The rash or irritation has been there for more than two weeks with no improvement
- The itch is breaking your sleep or making it hard to focus during the day
- The skin is cracking, bleeding, or looking infected – warmth, swelling, and discharge are signs something more is going on
- Creams and moisturizers from the pharmacy haven’t helped
- Your nails are changing – pitting, thickening, or separating
- You have joint pain or morning stiffness alongside skin symptoms
- You have a diagnosis but the treatment prescribed isn’t doing what it should
- The condition is affecting how you feel about yourself, your sleep, your social life, or your work
Skin conditions don’t just stay on the skin. They affect sleep, mood, confidence, and daily function. A provider who actually listens to what you’re experiencing can make a significant difference – not just in your diagnosis, but in how manageable life feels afterward.
Get Support
Living with skin flares and not being sure what’s causing them is exhausting. At Wade’s Care First, Charles Wade FNP-BC, approaches dermatology the same way he approaches everything – by listening first. Not a quick glance and a prescription, but an actual conversation about what you’re experiencing and what’s been tried.
Same-day telehealth appointments are available in Arizona, Florida, Illinois, Indiana, Kentucky, Michigan, Nevada, New York, and Texas. You don’t need a referral. You don’t need to sit in a waiting room. You just need to book.
Visit wadescarefirst.com to schedule. Your skin has been waiting long enough.